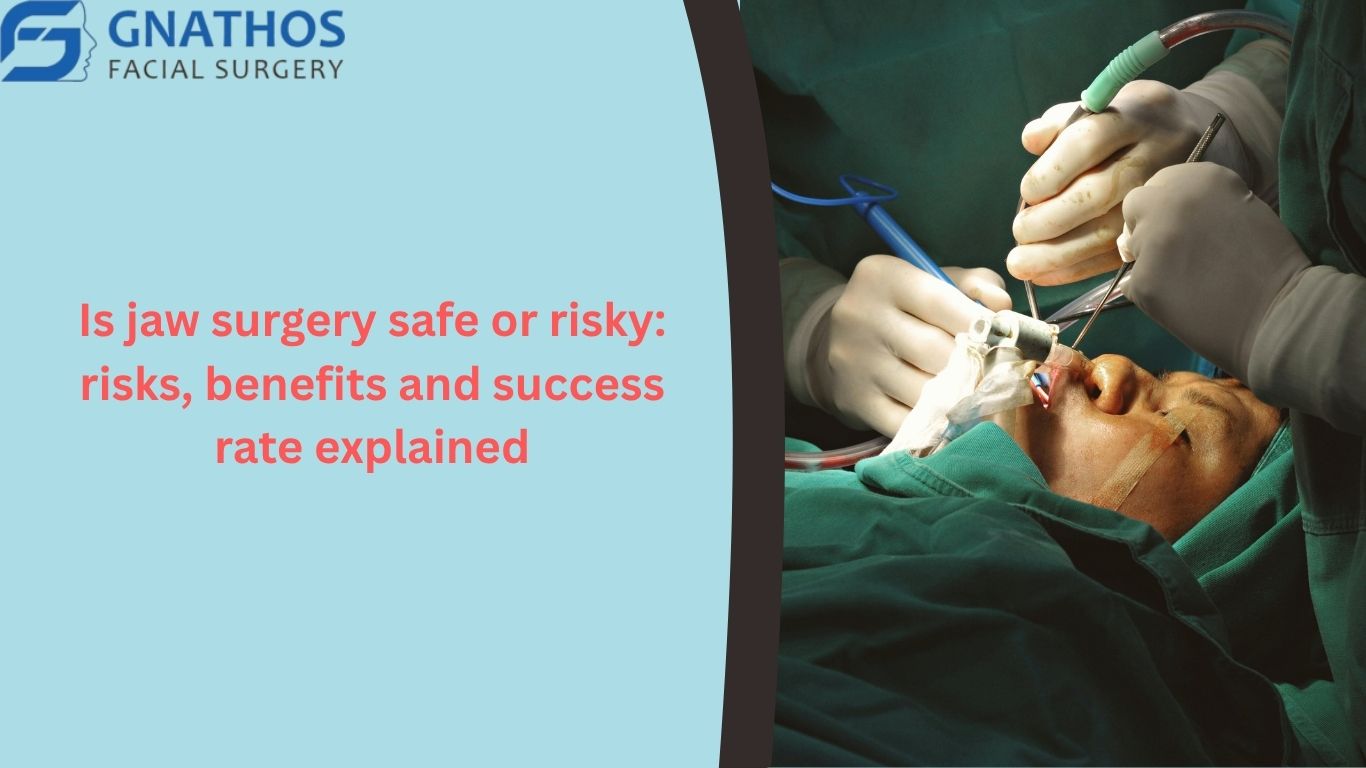
Are you struggling with chewing difficulties, chronic jaw pain, or severe sleep apnea? Perhaps your dentist or orthodontist has recommended orthognathic surgery to correct a severe overbite or underbite. But like anyone facing a major medical procedure, it is completely normal to ask: is jaw surgery safe or risky? It is a significant decision that involves balancing potential long-term health benefits with the temporary discomforts and surgical risks.
The good news is that modern medical advancements, 3D imaging, and specialized surgical techniques have made corrective jaw surgery highly successful and safer than ever before. In this comprehensive guide, we will break down the safety, risks, benefits, and overall success rate of jaw surgery to help you make an informed and confident choice about your facial health.
What is Orthognathic Surgery?
Commonly known as corrective jaw surgery, orthognathic surgery is a specialized procedure performed by an oral and maxillofacial surgeon to fix irregularities of the jaw bones. The main goal is to properly realign the upper jaw (maxilla) and the lower jaw (mandible) so they work together in harmony.
While many people mistakenly assume this procedure is purely cosmetic, it is fundamentally a functional surgery. It improves a patient’s ability to bite, talk, breathe, and chew. Because the jawbones dictate the lower structure of the face, moving them naturally results in improved facial symmetry and aesthetics as a secondary benefit.+1
Causes and Reasons: Why Do People Need Jaw Surgery?
In a perfectly developing body, the upper and lower jaws grow at the exact same rate. However, sometimes they develop at different speeds or in different directions, leading to severe misalignment. The most common reasons for requiring this surgery include:
- Genetics and Birth Defects: Congenital issues, such as a cleft lip or cleft palate, can significantly affect how the jaw bones grow over time.
- Facial Trauma: Severe accidents, sports injuries, or falls that cause facial fractures might require comprehensive jaw reconstruction to restore normal function.
- Severe Orthodontic Issues: When traditional braces alone cannot fix severe skeletal underbites, overbites, crossbites, or open bites.
- TMJ Wear and Tear: Chronic strain on the jaw joints can lead to debilitating conditions requiring surgical intervention.
Symptoms of Jaw Misalignment
How do you know if you are a candidate for orthognathic surgery? Jaw misalignment can cause both functional and aesthetic issues. Watch out for these common warning signs:
- Chronic difficulty with chewing, biting, or swallowing food.
- Persistent jaw pain, facial pain, or severe tension headaches.
- Excessive and uneven wear on your teeth.
- Breathing problems, including chronic mouth breathing, snoring, and obstructive sleep apnea.
- A visibly unbalanced facial appearance, such as a severely receding chin or a protruding lower jaw.
- Clicking, popping, or grating sounds in the jaw joint, which are strong indicators of TMJ disorder.
Diagnosis and Planning: Precision for Safety
Before answering the question—is jaw surgery safe or risky for your specific case—a specialist will conduct a thorough medical evaluation. The accuracy of the diagnosis directly influences the safety of the procedure.
The diagnostic and planning process usually involves:
- 3D CBCT Scans: These high-resolution scans provide a detailed, three-dimensional view of your facial bones, teeth, and crucial nerve pathways.
- Virtual Surgical Planning (VSP): This is where modern surgery shines. Advanced computer software allows the maxillofacial surgeon to digitally simulate the entire surgery beforehand. They can map out exact bone cuts and foresee outcomes, which significantly reduces surgical risks and improves the success rate.
- Dental Impressions: Molds of your teeth are taken to study your bite alignment and coordinate treatment with your orthodontist.
Common Jaw Treatment Options
Jaw surgery is highly customized to your specific skeletal needs. Depending on your diagnosis, your surgeon may recommend one or a combination of the following procedures:
- Maxillary Osteotomy (Upper Jaw Surgery): Often referred to as a Le Fort procedure, this is used to correct open bites, crossbites, or an upper jaw that recedes too far back. The surgeon moves the upper jaw forward, backward, or adjusts its angle.
- Mandibular Osteotomy (Lower Jaw Surgery): Commonly called a BSSO (Bilateral Sagittal Split Osteotomy), this technique fixes a severe underbite or overbite by moving the lower jawbone forward or backward.
- Bimaxillary Osteotomy (Double Jaw Surgery): In complex cases where both jaws are misaligned, the surgeon will reposition both the upper and lower jaws simultaneously.
- Genioplasty (Chin Surgery): This is often done alongside jaw surgery to correct a receding chin, providing better facial harmony and improving overall cosmetic facial surgery results.
Is Jaw Surgery Safe or Risky? Understanding the Balance
So, is jaw surgery safe or risky? Like all major surgeries performed under general anesthesia, it inherently comes with potential risks. However, when performed by a board-certified, highly trained maxillofacial surgeon in a modern facility, it is widely considered a highly safe procedure with an excellent success rate.
Let’s look at a clear comparison of the life-changing benefits versus the potential surgical risks.
Benefits vs. Risks of Jaw Surgery
| The Benefits (Why it is worth it) | The Risks (What to watch out for) |
|---|---|
| Enhanced Chewing & Digestion: Restores normal bite function, preventing tooth wear and digestive issues. | Infection: Rare, but possible at the incision sites inside the mouth. Managed with antibiotics. |
| Lasting Pain Relief: Relieves chronic TMJ pain, neck strain, and frequent headaches. | Nerve Damage: Temporary numbness in the chin, lips, or gums is common; permanent numbness is very rare. |
| Improved Breathing: Cures or greatly reduces obstructive sleep apnea and chronic snoring. | Swelling and Bleeding: Expected during the first few weeks of the recovery process. |
| Facial Harmony: Enhances facial symmetry, proportion, and significantly boosts self-confidence. | Relapse: The jaw may slightly shift back over time, though modern titanium plates make this extremely rare. |
| Speech Improvement: Fixes speech impairments (like lisps) caused by poor structural jaw alignment. | Bite Adjustment: You will likely need braces before and after the surgery to perfect the teeth alignment. |
Recovery and Prevention Tips
The ultimate success of your surgery heavily depends on your commitment to post-operative care. While complete bone healing takes 6 to 12 weeks, the initial, most intense recovery phase takes about 2 to 3 weeks.
Tips for a Smooth, Safe Recovery:
- Follow a Strict Liquid/Soft Diet: You will need to stick to smoothies, blended soups, and protein shakes for the first few weeks to avoid putting pressure on the healing jawbones.
- Use Ice Packs Consistently: Apply cold compresses to manage facial swelling during the critical first 48 to 72 hours.
- Maintain Meticulous Oral Hygiene: Keeping the surgical incisions clean is vital to prevent infection. You will use a prescribed antibacterial mouthwash since traditional brushing will be difficult early on.
- Rest with Your Head Elevated: Sleep with your head propped up on two or three pillows to minimize blood flow to the face and reduce swelling.
- Avoid Strenuous Activities: Skip heavy lifting, intense cardio, and contact sports for at least a month to six weeks to prevent jarring the jaw.
When to See a Doctor
Before surgery, you should seek immediate medical advice if you experience severe jaw locking, struggle to open or close your mouth, or have intense difficulty breathing while sleeping.
If you have already undergone the procedure, contact your oral surgeon immediately if you experience a high fever, excessive bleeding that does not stop with pressure, or sudden, severe pain that medication cannot control, as these could be signs of a post-surgical infection.
Conclusion
When asking yourself, is jaw surgery safe or risky, the answer largely depends on your specific diagnosis, your overall health, and the expertise of your surgical team. While the recovery process requires patience, proper nutrition, and commitment, the long-term benefits are profound. From pain-free chewing to clear breathing and beautifully enhanced facial confidence, orthognathic surgery is a life-changing procedure for most patients.
If you are dealing with a misaligned jaw, do not let fear of the unknown hold you back from a healthier, more comfortable life.
Ready to explore your options? Consult a specialist at Gnathos Face Surgery today to book an appointment and get a personalized, safe treatment plan tailored to your needs.
Frequently Asked Questions (FAQs)
Q: How painful is jaw surgery recovery? A: You will be under general anesthesia during the procedure, so you will not feel anything. Because the surgery is usually performed entirely inside the mouth, there are no external facial scars. Post-surgery pain is typically manageable with prescribed pain medication. Most patients report feeling intense pressure, discomfort, and swelling rather than sharp, severe pain.
Q: What is the success rate of orthognathic surgery? A: Jaw surgery has a remarkably high success rate, often exceeding 95% for improving function and aesthetics. Modern 3D imaging and virtual surgical planning have made the procedure incredibly precise, safe, and predictable.
Q: Will jaw surgery completely change my face? A: Yes, it will alter your appearance. Because the jawbones provide the foundational structure for the lower half of your face, moving them will change your profile. However, the changes are almost always positive, resulting in better facial symmetry, a stronger jawline, and a more balanced, natural look.+1
Q: Is jaw surgery safe or risky for older adults? A: Age alone does not disqualify someone from jaw surgery. While younger patients (late teens to early 30s) generally heal faster and have more adaptable bones, older adults can safely undergo the procedure if they are in good overall health. Your surgeon will carefully evaluate your bone density and medical history first.
Q: How long does it take to fully recover and see final results? A: The initial healing phase takes about 2 to 3 weeks, allowing most people to return to school or light work. However, complete bone healing can take up to 12 weeks. Residual swelling can take several months to completely resolve, which is when you will see your final facial results. The full orthodontic process (including braces) may continue for six months to a year post-surgery.+1
Q: Are there non-surgical alternatives to jaw surgery? A: In very mild cases, orthodontics (traditional braces or clear aligners) can correct minor bite issues by shifting the teeth. However, if the underlying problem is the skeletal structure of the jawbone itself, moving the teeth will not fix it. In these cases, orthognathic surgery is usually the only effective, long-term solution.