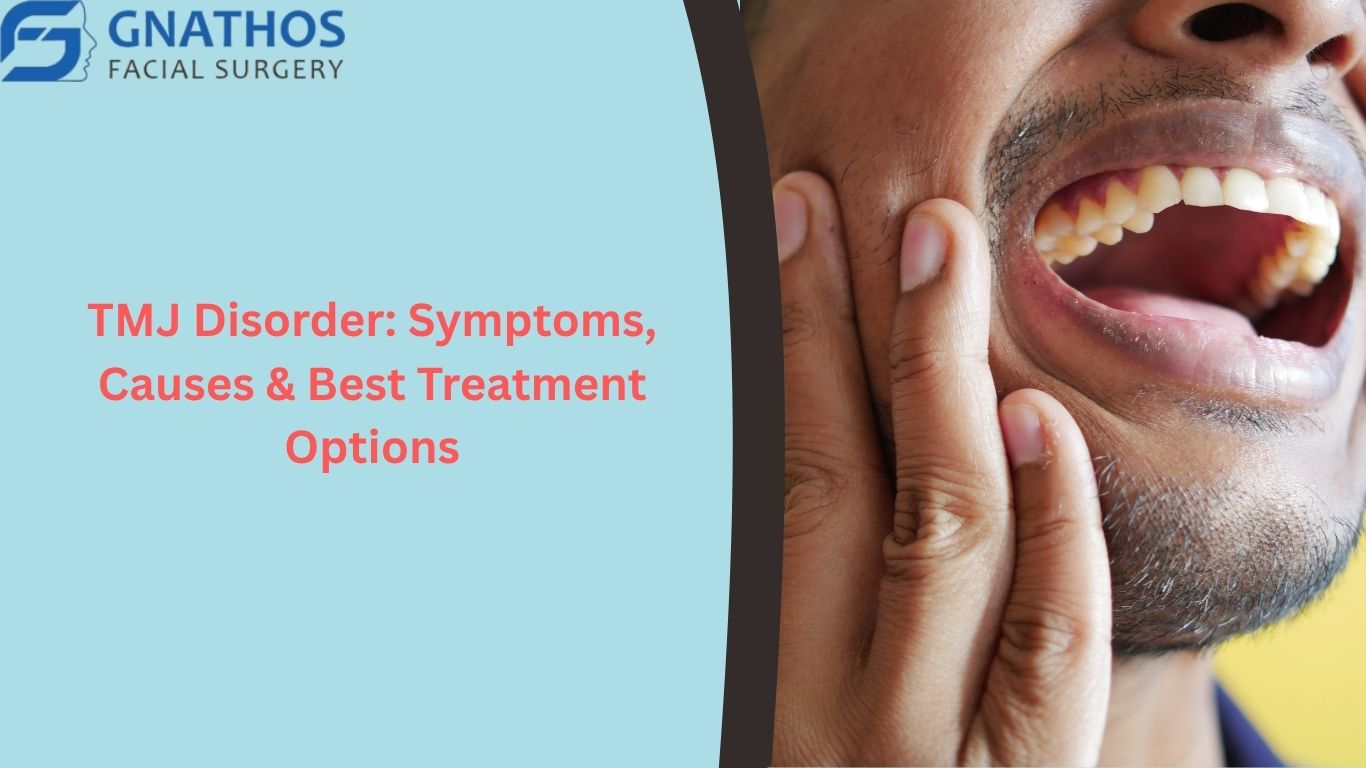
Do you experience a clicking sound when you chew, or find your jaw locking after a long day? If so, you might be suffering from TMJ Disorder. This condition affects the temporomandibular joint—the hinge that connects your jaw to your skull—and can cause debilitating pain that radiates through the face, neck, and head. While the discomfort can feel overwhelming, understanding the underlying causes and modern medical interventions can help you find lasting relief. This comprehensive guide explores everything from initial symptoms to the latest surgical and non-surgical solutions available today.
What is TMJ Disorder?
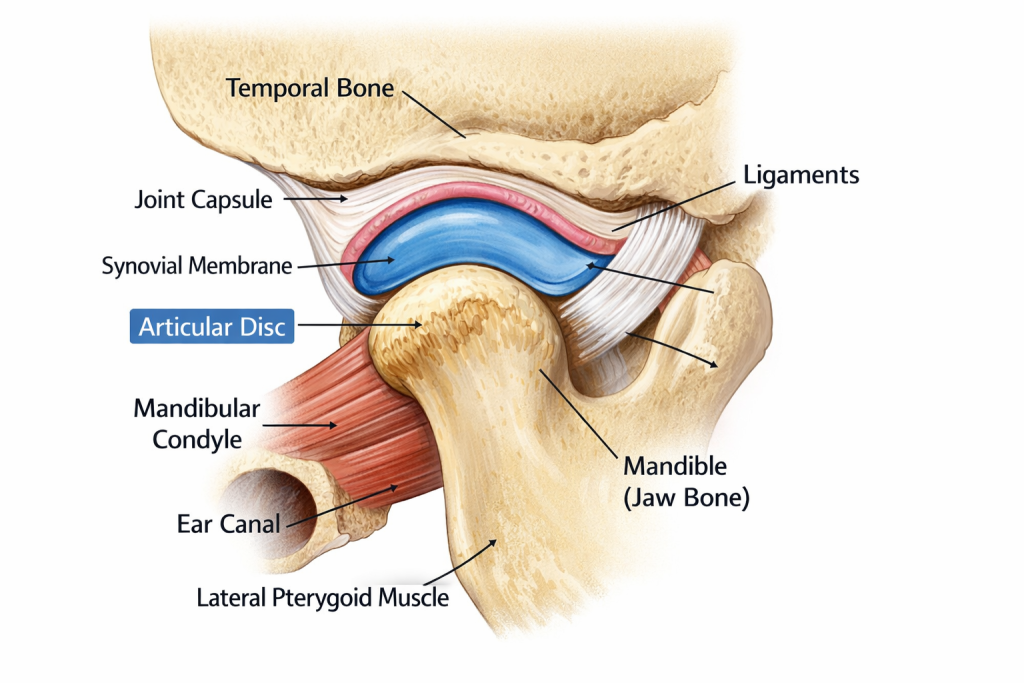
The temporomandibular joint (TMJ) is one of the most complex joints in the human body. It facilitates the sliding and rotating motions required for talking, chewing, and yawning. TMJ Disorder, often referred to as TMD, occurs when the joint or the surrounding muscles become inflamed or misaligned. Because this joint is used constantly throughout the day, even minor issues can escalate into significant chronic pain.
Common Causes and Reasons
There is rarely a single cause for jaw dysfunction; rather, it is often a combination of factors.
- Bruxism (Teeth Grinding): Constant clenching or grinding, especially during sleep, puts immense pressure on the joint.
- Physical Trauma: An injury to the jaw or the joint itself, such as a sports injury or accident, can lead to displacement.
- Arthritis: Osteoarthritis or rheumatoid arthritis can damage the cartilage that protects the joint.
- Misalignment: If the upper and lower teeth do not fit together properly (malocclusion), the joint must overcompensate.
- Stress: High levels of stress often lead to subconscious muscle tension in the face and neck.
Recognizing the Symptoms
Identifying TMJ Disorder early can prevent the condition from becoming chronic. Look for these warning signs:
- Jaw Pain or Tenderness: A persistent ache in the jaw area or near the ear.
- Clicking or Popping: A distinct sound when opening or closing the mouth.
- Limited Range of Motion: Difficulty opening the mouth wide or a “locking” sensation.
- Facial Aching: Pain that spreads to the cheeks or temples, often mistaken for a toothache.
- Ear Issues: Tinnitus (ringing in the ears) or a feeling of fullness without an infection.
Diagnosis: How Specialists Evaluate Your Jaw
At Gnathos Face, a proper diagnosis is the first step toward recovery. A specialist will typically perform:
- Physical Examination: Checking the range of motion and listening for joint sounds.
- Palpation: Pressing on the jaw muscles to identify trigger points of pain.
- Imaging Studies: Using Dental X-rays to view the teeth and bone structure.
- MRI or CT Scans: These provide detailed images of the joint’s disc and surrounding soft tissues to check for internal derangement.
Best Treatment Options for TMJ Disorder
Treatment plans are usually customized based on the severity of the misalignment and pain levels.
Non-Surgical Interventions
Most patients find relief through conservative methods:
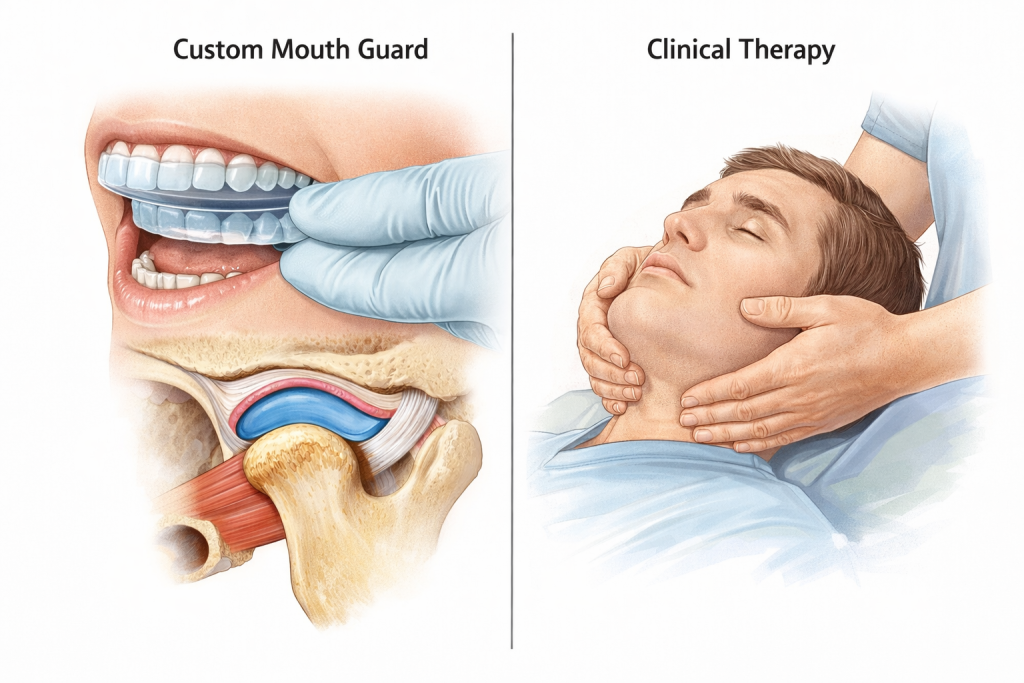
- Oral Splints or Mouth Guards: Custom-fit appliances worn at night to prevent grinding.
- Physical Therapy: Exercises to stretch and strengthen jaw muscles.
- Medications: Muscle relaxants, anti-inflammatories, or low-dose antidepressants to control pain.
Advanced and Surgical Procedures
When conservative treatments fail, more advanced Maxillofacial procedures may be necessary:
- Arthrocentesis: A minimally invasive procedure where fluid is used to wash out inflammatory byproducts from the joint.
- TMJ Arthroscopy: Using a small camera and instruments to perform minor repairs within the joint.
- Open-Joint Surgery: Reserved for structural issues or tumors within the joint.
- Corrective Jaw Surgery: In cases of severe malocclusion, Orthognathic surgery may be the permanent solution.
Comparison: Conservative vs. Surgical Treatment
| Feature | Conservative Management | Surgical Intervention |
|---|---|---|
| Goal | Pain relief & muscle relaxation | Structural repair & realignment |
| Recovery Time | Immediate (Ongoing) | 1 to 6 weeks |
| Invasiveness | Non-invasive | Minimally to highly invasive |
| Success Rate | High for muscular issues | High for structural damage |
Risks and Side Effects
Every medical procedure carries some risk. Non-surgical options like splints might feel uncomfortable initially. Surgical options carry risks typical of any procedure, such as temporary swelling, infection, or nerve sensitivity. It is essential to work with an experienced Oral and Maxillofacial Surgeon to minimize these risks and ensure the best outcome.
Recovery and Prevention Tips
Managing TMJ Disorder is a long-term commitment to joint health.
- Soft Food Diet: During flare-ups, stick to yogurt, mashed potatoes, and smoothies to rest the joint.
- Heat and Cold Packs: Use ice to reduce swelling and moist heat to relax tight muscles.
- Posture Correction: Avoid slouching, as neck tension directly impacts jaw alignment.
- Stress Management: Practice relaxation techniques or yoga to reduce jaw clenching.
When to See a Doctor
You should consult a specialist if your jaw pain is persistent or if you cannot open or close your mouth completely. Ignoring the signs can lead to permanent damage to the joint cartilage or chronic headaches. Seeking professional consultation early is the best way to avoid complex surgeries later.
Conclusion
Living with TMJ Disorder can be a daily struggle, affecting how you eat, speak, and smile. However, with the right combination of diagnostic precision and personalized care, relief is well within reach. From simple lifestyle adjustments to advanced reconstructive surgery, the goal is to restore your jaw’s natural function and eliminate pain. If you are tired of the clicking and the constant ache, take the first step toward a pain-free life today. Don’t let jaw pain control your life. Book an appointment with our experts at Gnathos Face and discover the best treatment path for your needs.
FAQ Section
Can TMJ Disorder go away on its own?
In some mild cases triggered by temporary stress, the symptoms may subside with rest and lifestyle changes. However, if the cause is structural or due to chronic grinding, professional intervention is required to prevent it from worsening.
Is TMJ surgery always necessary?
No. In fact, the majority of patients respond well to non-surgical treatments like splint therapy, physical therapy, and medication. Surgery is only considered when structural damage is present or conservative methods fail.
Can a dentist fix TMJ problems?
General dentists can often identify the signs and provide basic splints. However, complex cases should be managed by a specialist in Oral and Maxillofacial Surgery who has extensive training in the joint’s anatomy.
Does stress cause TMJ?
Stress is a major contributing factor. It often leads to jaw clenching and teeth grinding (bruxism), which puts excessive strain on the temporomandibular joint and surrounding muscles.
What foods should I avoid with TMJ?
Avoid hard, crunchy, or chewy foods like raw carrots, nuts, steak, and chewing gum. These require heavy jaw movement and can aggravate the joint during a flare-up.
Can TMJ cause ear pain?
Yes. Because the TMJ is located very close to the ear canal, inflammation in the joint is frequently felt as pain in or around the ear, even when no ear infection is present.